Last week, the internet told us about the “pill to cure Alzheimer’s”, which scientists had recently discovered. As usual, we can be safe in the knowledge that they found almost nothing of the sort.
HOWEVER, three studies published within the last couple of weeks have received far less attention despite pointing towards a simple way to reduce the risk of dementia in old age. It’s free, and everyone can do it. Sleep.
Alzheimer’s dementia takes a huge toll on both patients and their families, and is projected to soon cripple the Western healthcare systems that support them. Over 5 million people in the US live with Alzheimer’s, and within a few years, over a million people in the UK will have the disease. Alzheimer’s-related death rates continue to increase, while deaths from strokes, heart attacks and many forms of cancer are coming down.
By 2050, the cost of Alzheimer’s in the US is projected to be over $1 trillion per year (that’s 5% of US National debt), which doesn’t even include the billions saved through family caregivers looking after loved ones afflicted with this currently incurable disease.
It’s no wonder, then, that when rumours of a drug, which does something remotely related to Alzheimer’s and can be taken as a pill, enter the journalistic sphere, everybody gets into a frenzy.
Alzheimer’s dementia is a neurodegenerative disorder that is most commonly associated with memory problems, but also impacts mood, behavior and speech. Though the exact cause of Alzheimer’s isn’t fully understood, we know that the accumulation of damaged proteins in certain areas of the brain is intimately associated with the progression of the disease. When a brain cell (neuron) notices that there are all these bad proteins lying around, it turns off the machinery that normally makes new proteins as part of everyday cell function. The neuron assumes that there is a problem in the protein machinery, so shuts it down until the problem is fixed. Without the formation of new proteins, the neuron doesn’t make the normal things that are necessary for survival, and eventually dies.
As more neurons die, it causes a slow progression from mild cognitive impairment (MCI) through to the extensive late-stage brain atrophy that can be ultimately fatal.
A pill for Alzheimer’s?
The study that got everybody excited last week was based on an entirely different disease – prion disease. If that sounds familiar, prion diseases include BSE and CJD, which dominated the media in the late 1990’s. Prion diseases are also associated with the accumulation of protein in the brain (prion protein), and turn on the same “protective” mechanisms described above.
A group of scientists infected mice with prion proteins, and then treated them with a molecule that stops the cell turning off its protein-making machinery. These mice then had fewer signs of disability and memory loss compared to those that got a placebo treatment, despite prion proteins continuing to accumulate in the brain.
Now, there isn’t much money to be made from prion diseases, so the company that created this drug (called “GSK2606414”, since you asked) would probably be keen to make it relevant to Alzheimer’s, which has a much larger potential patient base. Could that be why there was a lot of media attention hailing a potential new Alzheimer’s treatment? I speculate.
However, even the Alzheimer’s societies have had to be reticent about the study, and admitted that any potential treatment for humans is still decades off. Here’s why:
Like we don’t have enough diabetes already…
We often hear sensationalised stories like this one, and it’s becoming harder to get excited about them. It is certainly very important that research like this continues, but wouldn’t it make sense to try and prevent the build-up of these abnormal proteins in the first place, rather than mitigate the effects once it’s probably already too late?
While you sleep, your brain clears out the junk
A paper published in Science three weeks ago gives us some clues as to how our brains do their housework. If you spend all day looking at brains, like I do, this is pretty cool. What these guys found was that, when mice are asleep, their brains shrink slightly. This provides more space for the fluid around the brain (cerebro-spinal fluid, or CSF) to circulate and remove waste products.
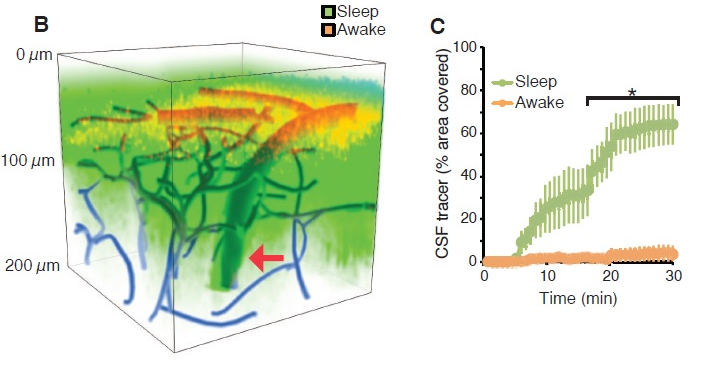
By injecting a substance that could be traced through the body, these researchers showed that new CSF is produced very slowly whilst we’re awake, but production and flow of CSF increases by more than 60% when we’re asleep.
One of the main “bad” proteins that accumulates in Alzheimer’s Disease is beta-amyloid (Aβ). Even in healthy people, Aβ proteins build-up in the brain during the day. The theory is that purely being awake, and the amount of brain power it requires, produces Aβ as a by-product, which will then need to be disposed of. The study found that Aβ protein was cleared from the brains of sleeping mice more over 100% faster than awake mice. As we make our CSF and handle waste from the brain in broadly the same way that mice do, we can expect similar results in humans.
HOWEVER, three studies published within the last couple of weeks have received far less attention despite pointing towards a simple way to reduce the risk of dementia in old age. It’s free, and everyone can do it. Sleep.
Alzheimer’s dementia takes a huge toll on both patients and their families, and is projected to soon cripple the Western healthcare systems that support them. Over 5 million people in the US live with Alzheimer’s, and within a few years, over a million people in the UK will have the disease. Alzheimer’s-related death rates continue to increase, while deaths from strokes, heart attacks and many forms of cancer are coming down.
By 2050, the cost of Alzheimer’s in the US is projected to be over $1 trillion per year (that’s 5% of US National debt), which doesn’t even include the billions saved through family caregivers looking after loved ones afflicted with this currently incurable disease.
It’s no wonder, then, that when rumours of a drug, which does something remotely related to Alzheimer’s and can be taken as a pill, enter the journalistic sphere, everybody gets into a frenzy.
Alzheimer’s dementia is a neurodegenerative disorder that is most commonly associated with memory problems, but also impacts mood, behavior and speech. Though the exact cause of Alzheimer’s isn’t fully understood, we know that the accumulation of damaged proteins in certain areas of the brain is intimately associated with the progression of the disease. When a brain cell (neuron) notices that there are all these bad proteins lying around, it turns off the machinery that normally makes new proteins as part of everyday cell function. The neuron assumes that there is a problem in the protein machinery, so shuts it down until the problem is fixed. Without the formation of new proteins, the neuron doesn’t make the normal things that are necessary for survival, and eventually dies.
As more neurons die, it causes a slow progression from mild cognitive impairment (MCI) through to the extensive late-stage brain atrophy that can be ultimately fatal.
A pill for Alzheimer’s?
The study that got everybody excited last week was based on an entirely different disease – prion disease. If that sounds familiar, prion diseases include BSE and CJD, which dominated the media in the late 1990’s. Prion diseases are also associated with the accumulation of protein in the brain (prion protein), and turn on the same “protective” mechanisms described above.
A group of scientists infected mice with prion proteins, and then treated them with a molecule that stops the cell turning off its protein-making machinery. These mice then had fewer signs of disability and memory loss compared to those that got a placebo treatment, despite prion proteins continuing to accumulate in the brain.
Now, there isn’t much money to be made from prion diseases, so the company that created this drug (called “GSK2606414”, since you asked) would probably be keen to make it relevant to Alzheimer’s, which has a much larger potential patient base. Could that be why there was a lot of media attention hailing a potential new Alzheimer’s treatment? I speculate.
However, even the Alzheimer’s societies have had to be reticent about the study, and admitted that any potential treatment for humans is still decades off. Here’s why:
- Prion diseases have a very different cause and disease progression compared to Alzheimer’s.
- Mouse models are often very poor mimics of disease processes in humans, and these mice were even genetically bred to make them more susceptible to prior disease.
- Mice that were already suffering from memory loss did not regain their memory. This would mean any future pill would have to be taken before any real symptoms of Alzheimer’s appear.
- Mice given the drug lost weight and had to be put-down early. Healthy mice don’t lose weight.
- Mice given GSK2606414 also had evidence of high blood sugar (a precursor to diabetes), after only five weeks of treatment, due to damage to the pancreas.
Like we don’t have enough diabetes already…
We often hear sensationalised stories like this one, and it’s becoming harder to get excited about them. It is certainly very important that research like this continues, but wouldn’t it make sense to try and prevent the build-up of these abnormal proteins in the first place, rather than mitigate the effects once it’s probably already too late?
While you sleep, your brain clears out the junk
A paper published in Science three weeks ago gives us some clues as to how our brains do their housework. If you spend all day looking at brains, like I do, this is pretty cool. What these guys found was that, when mice are asleep, their brains shrink slightly. This provides more space for the fluid around the brain (cerebro-spinal fluid, or CSF) to circulate and remove waste products.
By injecting a substance that could be traced through the body, these researchers showed that new CSF is produced very slowly whilst we’re awake, but production and flow of CSF increases by more than 60% when we’re asleep.
One of the main “bad” proteins that accumulates in Alzheimer’s Disease is beta-amyloid (Aβ). Even in healthy people, Aβ proteins build-up in the brain during the day. The theory is that purely being awake, and the amount of brain power it requires, produces Aβ as a by-product, which will then need to be disposed of. The study found that Aβ protein was cleared from the brains of sleeping mice more over 100% faster than awake mice. As we make our CSF and handle waste from the brain in broadly the same way that mice do, we can expect similar results in humans.
We know that the brain produces a number of waste products while you’re awake and, once these accumulate to a high enough concentration, they make you feel sleepy. It seems that, much like the effort it takes to use your brain while you’re awake, it also takes a lot of energy to get rid of all the waste that your brain produces. Therefore, your brain can only afford to do that while it’s asleep.
If you ignore signals to sleep, these waste products can actually force your brain to shut down small segments at a time, and this is thought to be why our mental performance can decrease so rapidly when we’re tired. Though the brain can handle short periods of sleep deprivation, it seems that sleeping too little for long periods of time may cause the irreversible build-up of damaging proteins.
Sleep more, remember more
If that wasn’t enough for you, two more studies came out in October, published in the well-respected journal JAMA Neurology, which support the theory of sleep (or the lack thereof) in the process of Alzheimer’s disease:
These are only small studies, and do include some potentially unreliable data, such as that from sleep questionnaires. However, if sleeping an extra hour a night will stop the inexorable march of a disease which could ruin whole economies, isn’t that worth a LOT of further research?
Don’t wait for the pill that may never come
It’s becoming more and more obvious that simply improving the way we look after ourselves will determine how long we live, and how long we will remember for. Any pill that comes out will only affect a disease that we may have been able to prevent all along, and the only person that can change that is you.
Of course, there are other factors which may increase your risk of Alzheimer’s, but there are also a huge number of benefits that come from sleeping more. I’ll save those for another time.
If you ignore signals to sleep, these waste products can actually force your brain to shut down small segments at a time, and this is thought to be why our mental performance can decrease so rapidly when we’re tired. Though the brain can handle short periods of sleep deprivation, it seems that sleeping too little for long periods of time may cause the irreversible build-up of damaging proteins.
Sleep more, remember more
If that wasn’t enough for you, two more studies came out in October, published in the well-respected journal JAMA Neurology, which support the theory of sleep (or the lack thereof) in the process of Alzheimer’s disease:
- Brain imaging in a group of people over 50 years-old showed that shorter sleep duration or worse quality of sleep was associated with more Aβ in the brain. This was highest in those sleeping fewer the 6 hours per night, and lowest in those sleeping more than 7 hours per night.
- In those with the apolipoprotein E ε4 gene (the strongest known genetic predisposition to Alzheimer’s), those experiencing the most restful sleep (measured by looking at sleep activity over 10 nights) had their risk of developing Alzheimer’s reduced by more than 50% over 6 years.
These are only small studies, and do include some potentially unreliable data, such as that from sleep questionnaires. However, if sleeping an extra hour a night will stop the inexorable march of a disease which could ruin whole economies, isn’t that worth a LOT of further research?
Don’t wait for the pill that may never come
It’s becoming more and more obvious that simply improving the way we look after ourselves will determine how long we live, and how long we will remember for. Any pill that comes out will only affect a disease that we may have been able to prevent all along, and the only person that can change that is you.
Of course, there are other factors which may increase your risk of Alzheimer’s, but there are also a huge number of benefits that come from sleeping more. I’ll save those for another time.
There are some basic rules that anybody can follow in order to improve their sleep quality:
All these methods have been shown to improve sleep, and are relatively easy. Your body naturally wakes up once it has sorted through all the memories and waste products from the previous day, so try and let that happen as frequently as possible. For most people that should be 7-8 hours.
Is it worth sleeping six hours a night if you’re going to perform less well, and then forget it all a few years later?
References:
1. Alzheimer’s Association - Alzheimer's Facts and Figures [http://www.alz.org/alzheimers_disease_facts_and_figures.asp]
2. Alzheimer’s Society – Statistics [http://www.alzheimers.org.uk/statistics]
3. Moreno JA, Halliday M, Molloy C, Radford H, Verity N, Axten JM, Ortori CA, Willis AE, Fischer PM, Barrett DA, Mallucci GR. Oral treatment targeting the unfolded protein response prevents neurodegeneration and clinical disease in prion-infected mice. Sci Transl Med. 2013 Oct 9;5(206):206ra138.
4. Faux NG, Ritchie CW, Gunn A, Rembach A, Tsatsanis A, Bedo J, Harrison J, Lannfelt L, Blennow K, Zetterberg H, Ingelsson M, Masters CL, Tanzi RE, Cummings JL, Herd CM, Bush AI. PBT2 rapidly improves cognition in Alzheimer's Disease: additional phase II analyses. J Alzheimers Dis. 2010;20(2):509-16.
5. Xie L, Kang H, Xu Q, Chen MJ, Liao Y, Thiyagarajan M, O'Donnell J, Christensen DJ, Nicholson C, Iliff JJ, Takano T, Deane R, Nedergaard M. Sleep drives metabolite clearance from the adult brain. Science. 2013 Oct 18;342(6156):373-7.
6. Porkka-Heiskanen T, Zitting KM, Wigren HK. Sleep, its regulation and possible mechanisms of sleep disturbances. Acta Physiol (Oxf). 2013 Aug;208(4):311-28.
7. Spira AP, Gamaldo AA, An Y, Wu MN, Simonsick EM, Bilgel M, Zhou Y, Wong DF, Ferrucci L, Resnick SM. Self-reported Sleep and β-Amyloid Deposition in Community-Dwelling Older Adults. JAMA Neurol. 2013 Oct 21.
8. Lim AS, Yu L, Kowgier M, Schneider JA, Buchman AS, Bennett DA. Modification of the Relationship of the Apolipoprotein E ε4 Allele to the Risk of Alzheimer Disease and Neurofibrillary Tangle Density by Sleep. JAMA Neurol. 2013 Oct 21.
- Set a routine. Go to bed and wake up at the same time every day. The odd social engagement is clearly an allowable exception.
- Avoid computers and phones for at least an hour before bed, and keep them out of the bedroom. The stimulation and higher stress hormone levels they cause prevent proper sleep cycles.
- Meditate, de-stress, and make sure your bedroom is dark and a comfortable temperature.
- Short-term supplementation with melatonin (the body’s natural “sleep” hormone) or L-tryptophan (an amino acid) can help re-start a proper sleep pattern, and allow a more natural type of sleep compared to more conventional sleeping tablets.
All these methods have been shown to improve sleep, and are relatively easy. Your body naturally wakes up once it has sorted through all the memories and waste products from the previous day, so try and let that happen as frequently as possible. For most people that should be 7-8 hours.
Is it worth sleeping six hours a night if you’re going to perform less well, and then forget it all a few years later?
References:
1. Alzheimer’s Association - Alzheimer's Facts and Figures [http://www.alz.org/alzheimers_disease_facts_and_figures.asp]
2. Alzheimer’s Society – Statistics [http://www.alzheimers.org.uk/statistics]
3. Moreno JA, Halliday M, Molloy C, Radford H, Verity N, Axten JM, Ortori CA, Willis AE, Fischer PM, Barrett DA, Mallucci GR. Oral treatment targeting the unfolded protein response prevents neurodegeneration and clinical disease in prion-infected mice. Sci Transl Med. 2013 Oct 9;5(206):206ra138.
4. Faux NG, Ritchie CW, Gunn A, Rembach A, Tsatsanis A, Bedo J, Harrison J, Lannfelt L, Blennow K, Zetterberg H, Ingelsson M, Masters CL, Tanzi RE, Cummings JL, Herd CM, Bush AI. PBT2 rapidly improves cognition in Alzheimer's Disease: additional phase II analyses. J Alzheimers Dis. 2010;20(2):509-16.
5. Xie L, Kang H, Xu Q, Chen MJ, Liao Y, Thiyagarajan M, O'Donnell J, Christensen DJ, Nicholson C, Iliff JJ, Takano T, Deane R, Nedergaard M. Sleep drives metabolite clearance from the adult brain. Science. 2013 Oct 18;342(6156):373-7.
6. Porkka-Heiskanen T, Zitting KM, Wigren HK. Sleep, its regulation and possible mechanisms of sleep disturbances. Acta Physiol (Oxf). 2013 Aug;208(4):311-28.
7. Spira AP, Gamaldo AA, An Y, Wu MN, Simonsick EM, Bilgel M, Zhou Y, Wong DF, Ferrucci L, Resnick SM. Self-reported Sleep and β-Amyloid Deposition in Community-Dwelling Older Adults. JAMA Neurol. 2013 Oct 21.
8. Lim AS, Yu L, Kowgier M, Schneider JA, Buchman AS, Bennett DA. Modification of the Relationship of the Apolipoprotein E ε4 Allele to the Risk of Alzheimer Disease and Neurofibrillary Tangle Density by Sleep. JAMA Neurol. 2013 Oct 21.

 RSS Feed
RSS Feed